Abstract
INTRODUCTION
Migrant workers comprise about one-fifth of Singapore’s resident population and form a substantial and vital component of the nation’s workforce. However, limited data is available regarding the barriers that migrant workers face in accessing healthcare from the healthcare providers’ perspective.
METHODS
We conducted a survey on doctors working in four restructured hospitals in Singapore, to assess what they perceived to be barriers faced by migrant workers in accessing healthcare. We also assessed the doctors’ understanding of migrant-health-related policies in Singapore.
RESULTS
A total of 427 survey responses were collected. Most respondents were senior doctors (senior residents or consultants) who had been practising medicine for a median of ten years. Among doctors, the most common perceived barriers to migrant workers accessing healthcare were related to culture/language (92.3%) and finances (healthcare cost) (81.0%). Of the six questions asked pertaining to migrant healthcare policy in Singapore, the respondents achieved a median of four correctly answered questions (interquartile range 3–5), and about 55% were unaware or unsure of available resources for migrant workers.
CONCLUSION
Our study identified healthcare providers’ perceived barriers to the delivery of healthcare to migrant workers, which corroborate previously published data reported by migrant workers themselves. Further efforts should be directed towards diminishing these barriers and increasing the literacy of migrant health among healthcare workers.
INTRODUCTION
Low-wage migrant workers in Singapore make up a large proportion of our population. As of December 2016, there were 1.15 million foreign workers holding either a Work Permit (workers in construction, manufacturing, marine/shipyard, process or service industries) or an S Pass (mid-level skilled workers).(1) This was approximately one-fifth of Singapore’s population of 5.5 million people.(2)
However, migrant workers are not entitled to the healthcare subsidies provided by the Singapore government, and do not qualify for the financing schemes available to Singaporeans and permanent residents.(3) Currently, under the Employment of Foreign Manpower Act, employers of low-wage migrant domestic and non-domestic workers are mandated by law to provide medical insurance coverage of at least SGD 15,000 a year for inpatient fees and day surgeries.(4) In addition, employers of migrant workers holding a Work Permit or S Pass are required legally to bear the costs of the provision of adequate medical treatment.(4) Technically, this should include outpatient care, and employers are expected to bear the costs when expenses are in excess of insurance coverage for inpatient care. Co-payment by the migrant worker may be permissible if certain conditions are met: medical treatment is not for work-related injuries; the co-pay amount is reasonable and does not exceed 10% of the worker’s monthly salary; duration of co-payment does not exceed six months; and the co-payment option is explicitly in the employment contract or collective agreement and has the worker’s full consent.(4,5) Healthcare costs due to injuries sustained during work are covered under the Work Injury Compensation Act (WICA), which mandates employers to purchase work injury compensation insurance for workers doing manual work (regardless of salary level) and for workers doing non-manual work with a salary of SGD 1,600 or less, with a minimum medical expenses coverage of SGD 36,000 a year.(6)
Despite the above policies, our recent survey of non-domestic migrant workers suggests that significant gaps still remain, resulting in significant barriers to accessing healthcare for migrant workers; furthermore, many had poor knowledge regarding their healthcare coverage and had experienced financial barriers in accessing healthcare.(7) Migrant workers often bear the costs of, or face barriers in outpatient care; inpatient insurance coverage may also be easily breached in the face of catastrophic illness.(7) Our survey’s findings were similar to those of a study by Lee et al, which reported poor knowledge about health-related insurance among male migrant workers and a greater likelihood for lower-income workers to delay or avoid seeking medical attention due to financial concerns.(8) However, these studies surveyed migrant workers who were largely well, with few having encountered major medical illnesses or hospitalisations. There is limited data on the experience of low-wage migrant workers within the tertiary healthcare setting, and the challenges faced by those who require hospitalisation or specialist care. Some of the challenges faced by migrant workers in Singapore have been highlighted by several reports published in the media, most of which revolve around the topic of inadequate issuance of sick leave to migrant workers(9,10) or of workers avoiding care due to cost concerns.(11) In 2012, Johnraj et al used the case studies of two low-wage migrant workers who had suffered catastrophic work injuries to illustrate the inadequacies of the WICA.(11)
Given the current paucity of information, particularly from the physician’s perspective, regarding potential barriers to care that low-wage migrant workers may experience in Singapore, and to complement our data pertaining to such barriers from the worker’s perspective,(7) we conducted a survey of doctors working in the tertiary care setting in Singapore to assess these barriers and to better understand potential factors affecting the care of migrant workers. As doctors play a large role in acting as healthcare advocates for their patients, we also assessed their understanding of migrant-health related policies in Singapore.
METHODS
Survey questions (
Table I
Online survey administered to doctors working in tertiary institutions in Singapore.
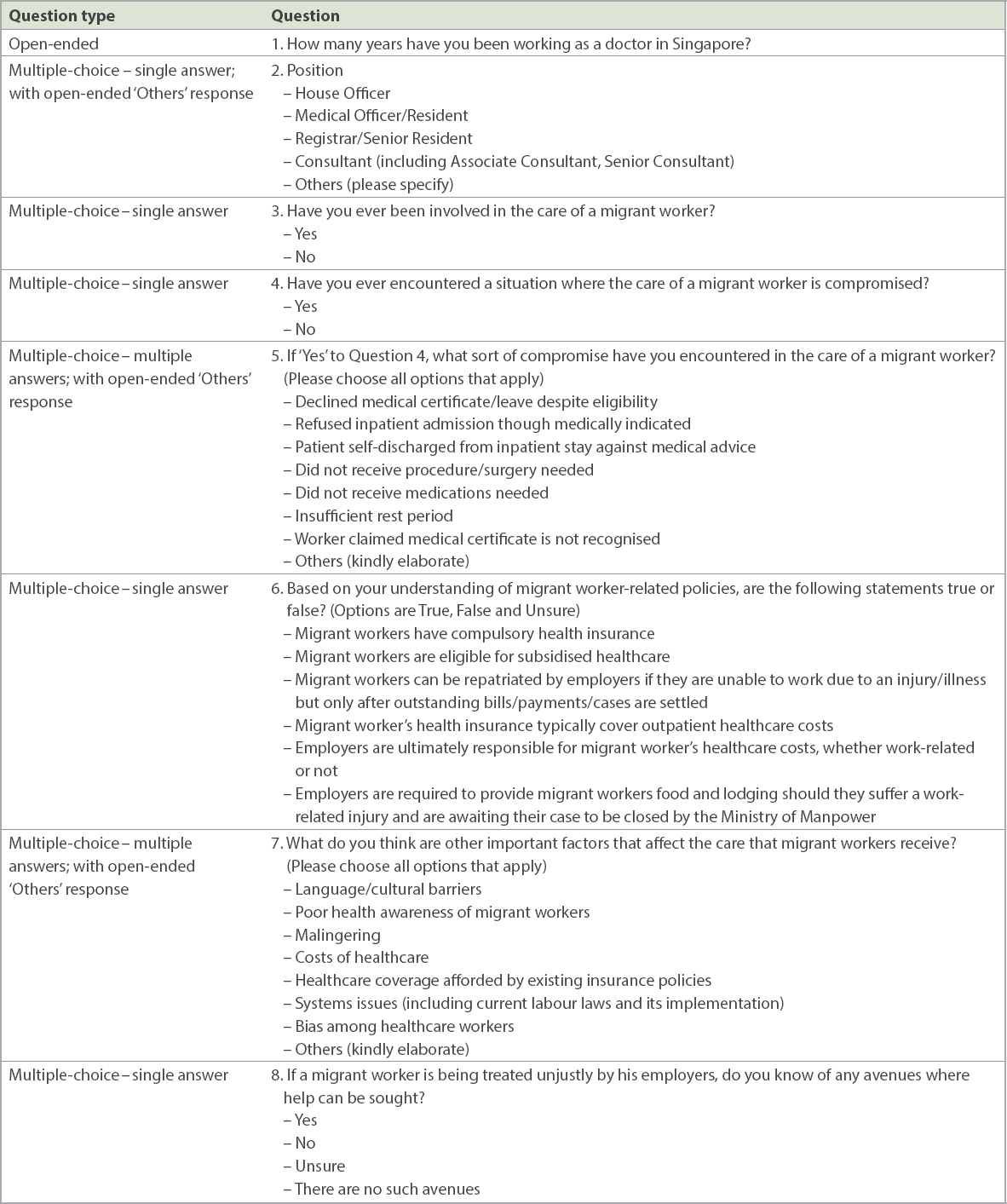
Questions were uploaded to an online survey site (
RESULTS
A total of 427 survey responses were collected between 18 August 2016 and 6 March 2017. The median number of years that respondents had worked as doctors in Singapore was 10 (interquartile range [IQR] 6 –15) years (
Table II
Demographics of respondents in online survey of Singapore doctors working in tertiary institutions (n = 427).
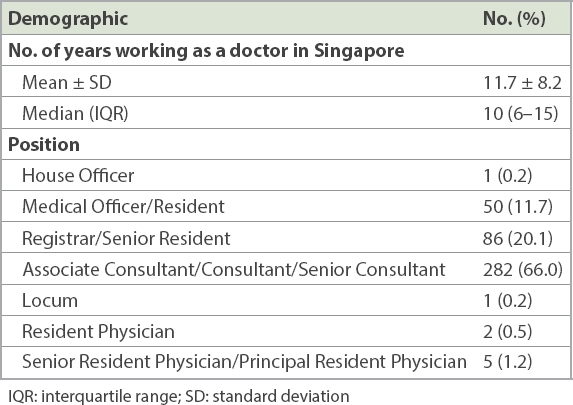
Almost all our respondents indicated that they had ever been involved in the care of migrant workers (n = 408, 95.6%;
Table III
Experience with care of migrant workers among Singapore doctors working in tertiary institutions: results of online survey.
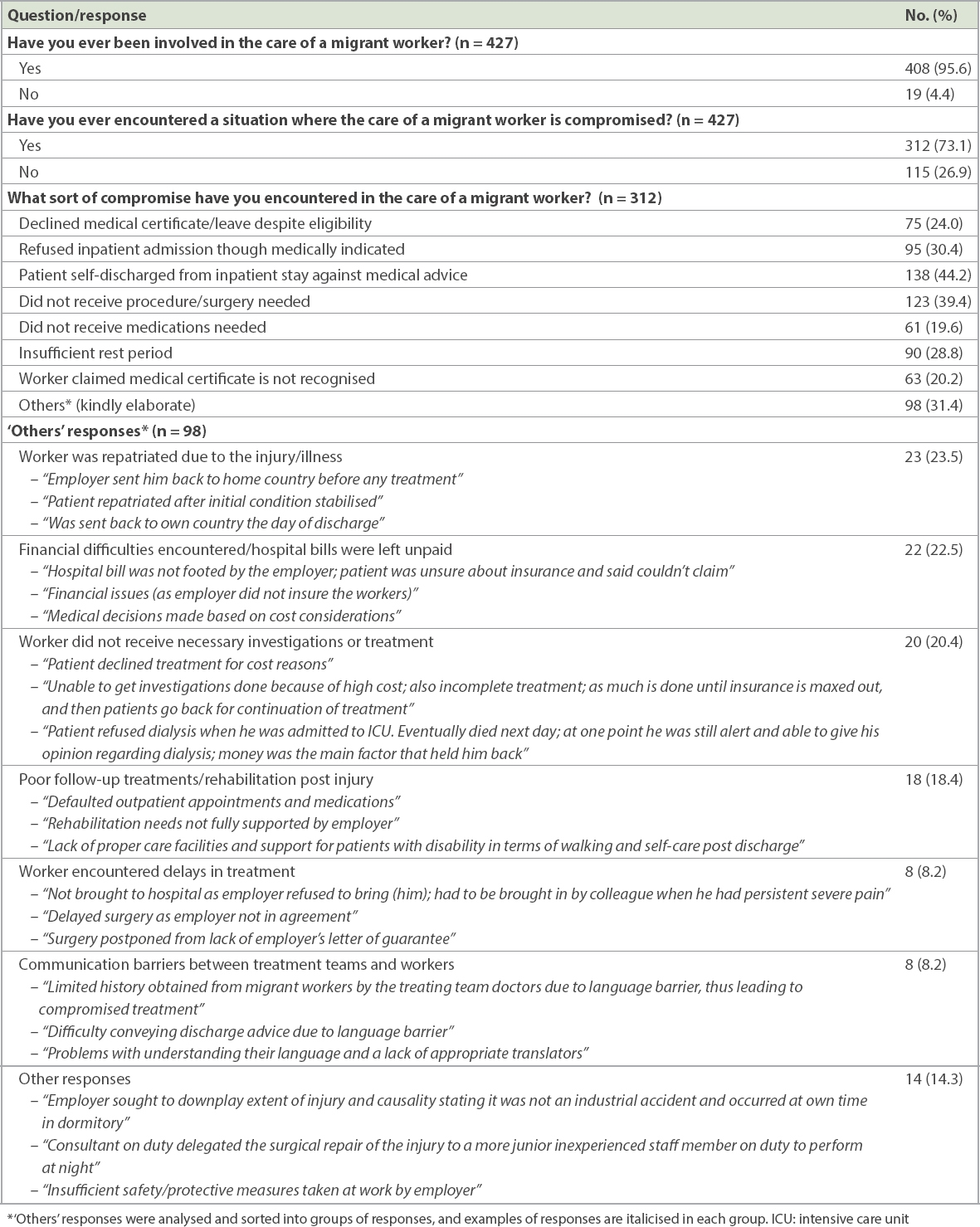
The most commonly highlighted factors that affected the care provided to migrant workers (
Table IV
Factors affecting care of migrant workers identified by Singapore doctors working in tertiary institutions: results of online survey.
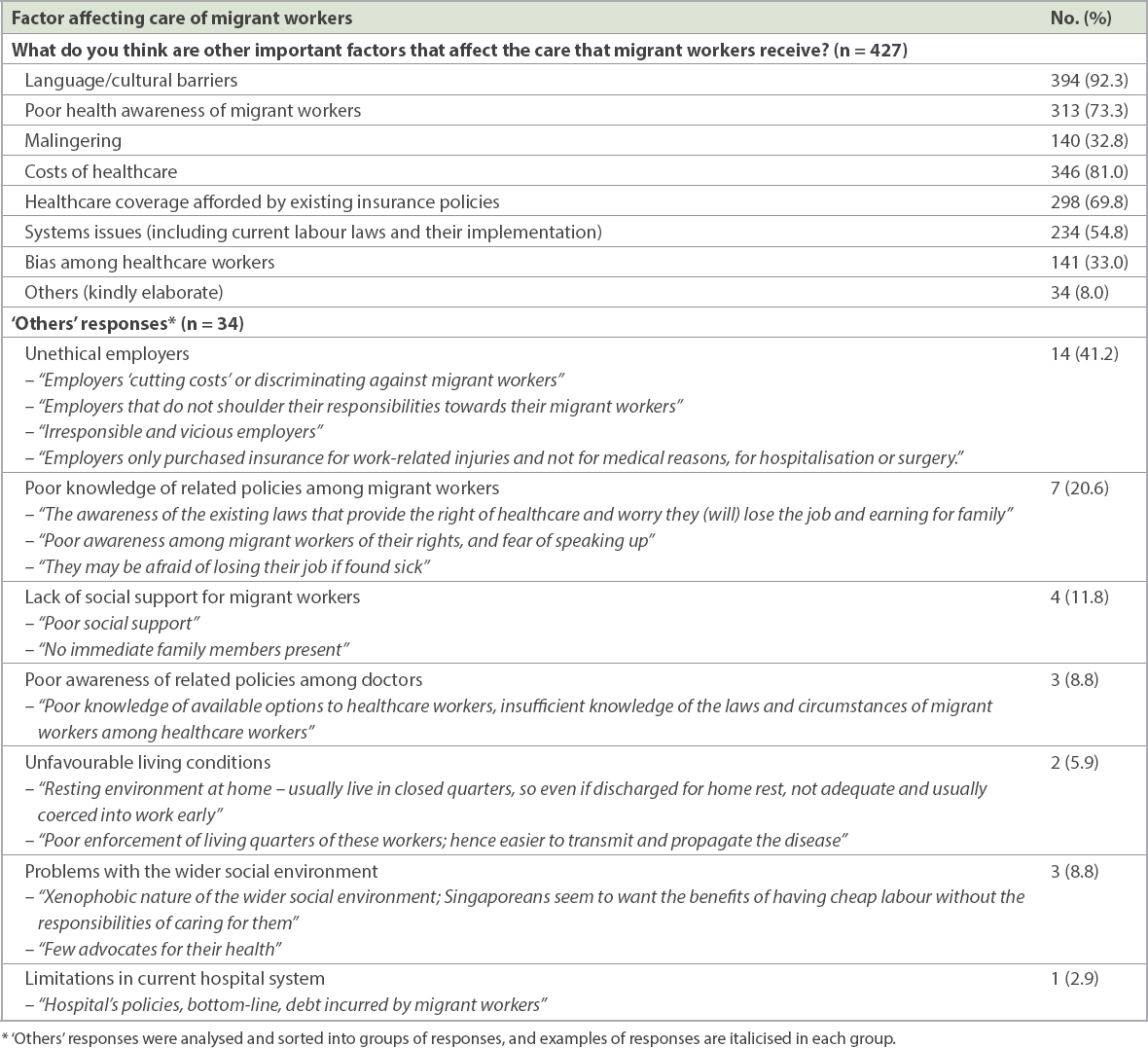
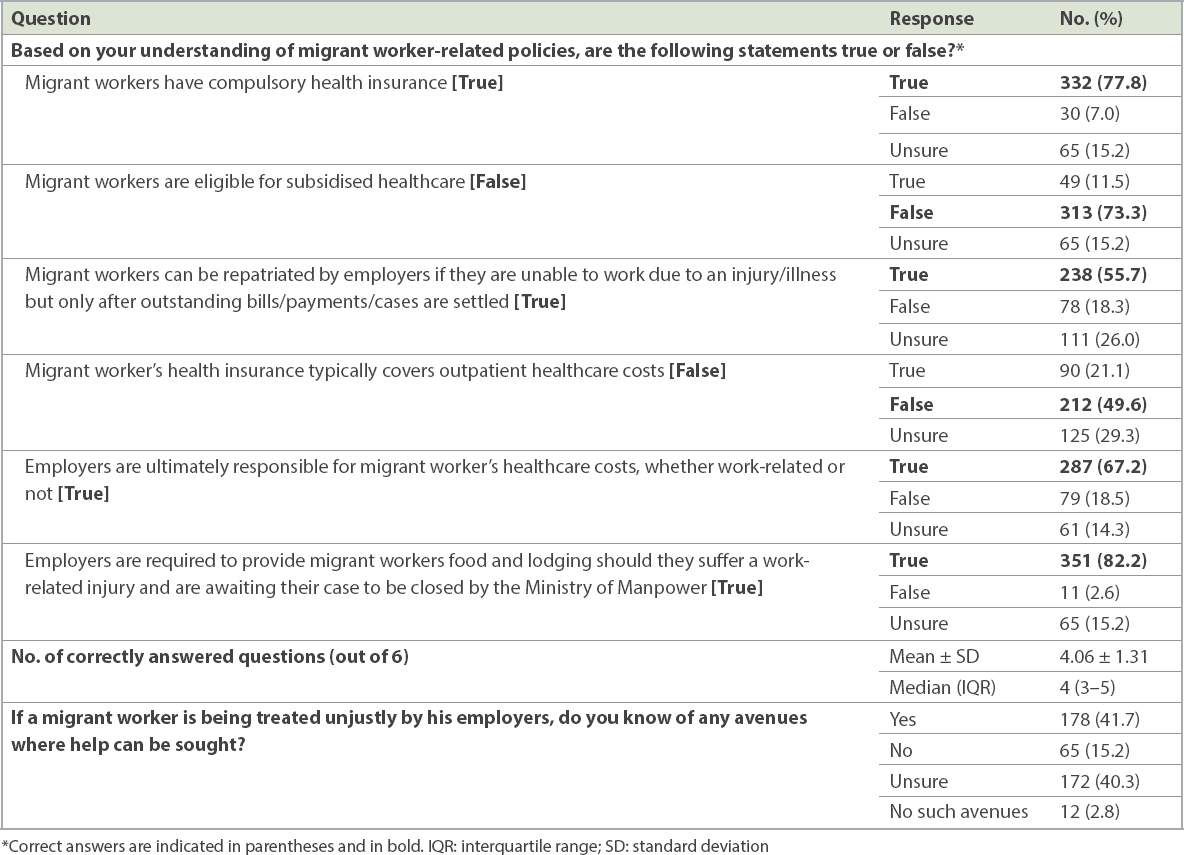
The percentage of doctors who selected correct responses for each of the six questions asked regarding migrant health policies (
Table V
Assessment of knowledge of migrant health policies among Singapore doctors working in tertiary institutions: results of online survey.
DISCUSSION
Migrants all over the world face various challenges as they transit and adapt to their receiving countries. Among these challenges are barriers to healthcare, which may be accentuated by cultural, language and socioeconomic factors, which may also vary depending on the healthcare policy and provisions in the receiving country. Singapore is a small city-state country that is highly dependent on migrant labour for its economic well-being. While official statistics on a per-country basis are not published by the Ministry of Manpower, the majority of migrant workers in Singapore hail from South India, Bangladesh and China.(7) While most migrant workers in Singapore are relatively young when they arrive,(7) migrant workers from these countries may stay in Singapore for up to 14–26 years,(12) and a substantial proportion of them go on to develop chronic diseases, such as hypertension and diabetes mellitus, and their attendant complications. Over the years, we have witnessed an increasing burden of chronic diseases at charity clinics serving these migrant workers (based on unpublished data from HealthServe and Karunya Community Clinics). Migrant workers in Singapore are also at risk of various occupational diseases (including work injuries, which can be life- or limb-threatening)(13) and various infectious diseases by virtue of their countries of origin, housing conditions or other behavioural factors.(14,15)
Data from this current survey on migrant worker healthcare, which was conducted among doctors from various restructured public hospitals, provides a parallel perspective and corroborates our survey findings of the migrant workers themselves.(7) Three main findings were gleaned from the current survey.
Firstly, culture and language remain significant healthcare barriers (92.3% of doctor-respondents). Navigating a complex medical system may be challenging for migrants due to language and cultural differences. Knowledge about healthcare coverage or entitlements may also be impaired because of a lack of clear information in their native language, especially if the details are not communicated clearly at the point of employment. In our previous survey among 433 non-domestic migrant workers, 22% were unsure if they had medical insurance coverage, and of those who knew they were insured, 60% were unsure if their insurance coverage included inpatient or outpatient costs. 73% reported not having received any insurance coverage information from their employers; of the 65 (15%) who did, only 21 (32%) received the information in their native language.(7) Efforts should be directed towards improving migrant workers’ understanding of healthcare provisions mandated by law and ensuring that insurance information is provided in the worker’s native language. Better delivery of healthcare information, including the wider use of educational materials in various languages spoken by migrants and more widespread use of language interpretation services (where appropriate), as well as continued education of healthcare providers to equip them to deliver culturally sensitive care, are important areas to focus on.
Secondly, financial factors pose a significant barrier to the delivery of healthcare to migrants. In the current study, 73.1% of doctor respondents reported encountering situations where healthcare delivery to a migrant worker was compromised, with financial barriers cited as a significant factor by 81.0% of respondents. In our recent companion survey among migrants,(7) 22% reported financial barriers to accessing healthcare, and on multivariable analysis, this was associated with a 3.9 times increased risk of psychological distress. Contributors to financial barriers may include the general lack of a mechanism for outpatient subsidies/coverage for low-wage migrant workers, possible breach of insurance payouts in the face of catastrophic illness and debt-fuelled migration (which often starts in the workers’ country of origin). While these issues are not easily resolved, a multilateral approach involving policymakers in both the sending and receiving countries, employers and insurers is needed. Suggested priority areas for further study and/or intervention have been detailed in our previous work.(7) While some improvements have been made in healthcare policy for migrant workers in Singapore (such as compulsory medical insurance for inpatient care and day surgery, which saw the minimum coverage raised from SGD 5,000 to SGD 15,000 in 2008), our survey highlights remaining barriers in the delivery of healthcare to migrant workers, from a healthcare provider’s perspective. It is hoped that this study, coupled with the findings from our recent migrant worker survey(7) and other recent studies,(8) will provide further data for lawmakers to improve healthcare policy, delivery and regulatory enforcement for our migrant workers in Singapore.
Lastly, akin to the lack of knowledge among migrants about healthcare coverage eligibility, doctors themselves were somewhat deficient in their knowledge of migrant health policies in Singapore (
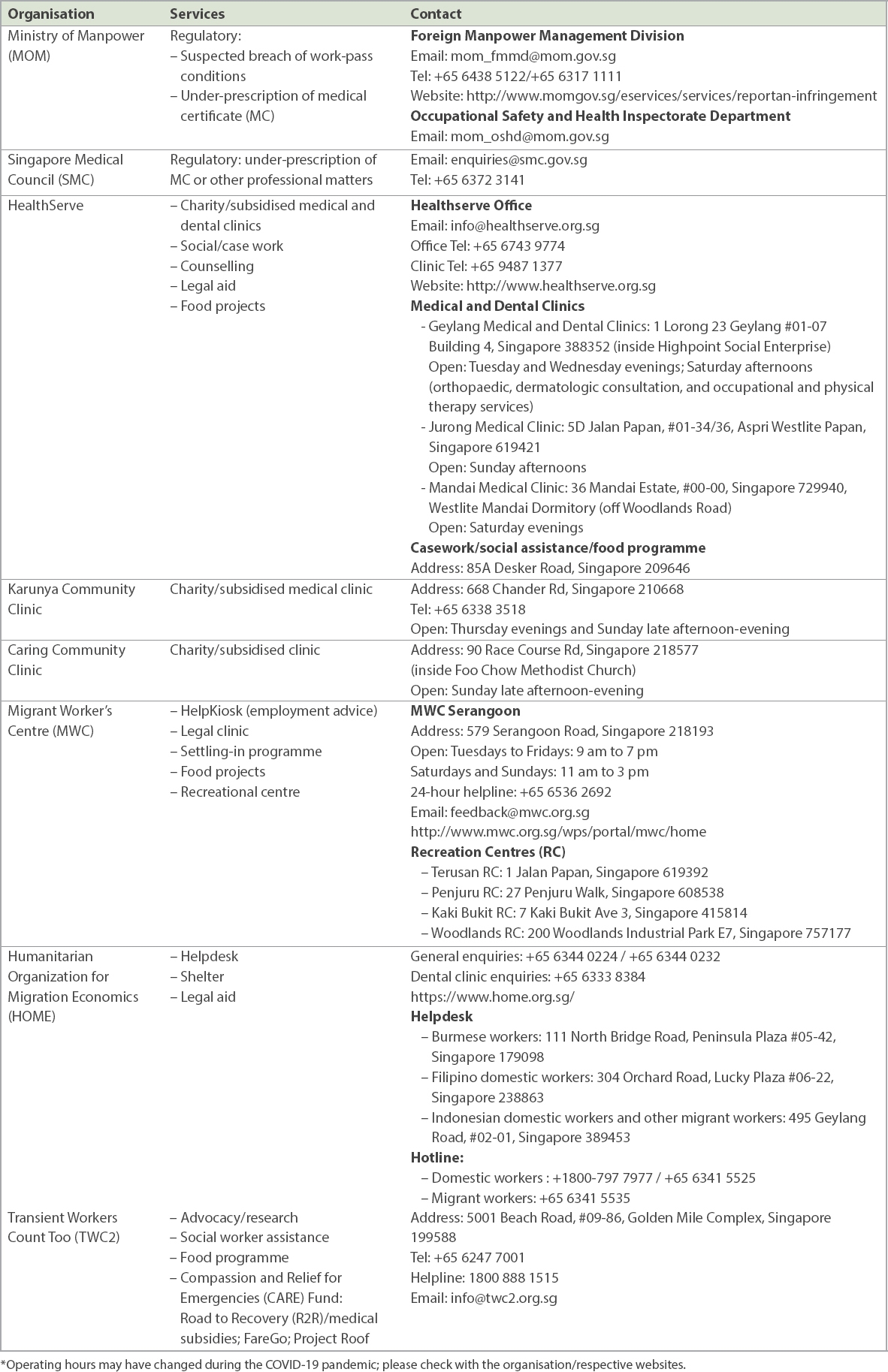
Table VI
Resources for migrant workers in Singapore.*
In conclusion, we identified various barriers to healthcare delivery to migrant workers in Singapore from the healthcare provider’s perspective. Among these, language/cultural and financial factors were cited as the most common barriers, but these are likely to be intertwined with multiple other factors such as prevailing healthcare policy, employer behaviour and the degree of knowledge/healthcare advocacy among healthcare providers. Further work is needed to overcome these barriers and improve migrant-health literacy among doctors, so that they may act as healthcare advocates for patients. In so doing, healthcare providers can contribute toward achieving universal health coverage and the promotion of a safe and secure working environment for all workers, as outlined in the United Nations (UN) 2030 Agenda for Sustainable Development (UN Sustainable Development Goals 3 and 8),(17) as well as creating a society where each migrant worker is valued and lives a life of dignity.
ACKNOWLEDGEMENTS
We would like to thank all the doctor-participants in this survey and the management of the various hospitals for their support of this survey.


