Abstract
INTRODUCTION
This study aimed to compare instrumental vaginal deliveries (IDs) and Caesarean sections (CSs) performed at full cervical dilatation, including factors influencing delivery and differences in maternal and neonatal outcomes.
METHODS
A retrospective review was conducted of patients who experienced a prolonged second stage of labour at Singapore General Hospital from 2010 to 2012. A comparison between CS and ID was made through analysis of maternal/neonatal characteristics and peripartum outcomes.
RESULTS
Of 253 patients who required intervention for a prolonged second stage of labour, 71 (28.1%) underwent CS and 182 (71.9%) underwent ID. 5 (2.0%) of the patients who underwent CS had failed ID. Of the maternal characteristics considered, ethnicity was significantly different. Induction of labour and intrapartum epidural did not influence delivery type. 70.4% of CSs occurred outside office hours, compared with 52.7% of IDs (p = 0.011). CS patients experienced a longer second stage of labour (p < 0.001). Babies born via CS were heavier (p < 0.001), while the ID group had a higher proportion of occipitoanterior presentations (p < 0.001). Estimated maternal blood loss was higher with CSs (p < 0.001), but neonatal outcomes were similar.
CONCLUSION
More than one in four parturients requiring intervention for a prolonged second stage of labour underwent emergency CS. Low failed instrumentation rates and larger babies in the CS group suggest accurate diagnoses of cephalopelvic disproportion. The higher incidence of CS after hours suggests trainee reluctance to attempt ID. There were no clinically significant differences in maternal and neonatal morbidity.
INTRODUCTION
The recent years have seen a worldwide increase in the rates of Caesarean deliveries.(1-4) This can be attributed to several reasons, including lower procedure-related risks, increasing incidence of maternal requests and multiple pregnancies due to advances in fertility treatment.(5,6) While these factors account for most of the rise in elective Caesarean sections (CSs), there has been a similar increase in the proportion of emergency CSs performed.(7)
Emergency CSs may be further categorised into those performed in either the first or second stage of labour, depending on whether there is an arrest of dilatation or arrest of descent. The first stage of labour is defined as the duration from the beginning of labour until full cervical dilatation, while the second stage of labour refers to the fetal descent and expulsive phase after reaching full cervical dilatation. In managing patients experiencing a prolonged second stage of labour, obstetricians are faced with the choice of two interventions: instrumental vaginal delivery (ID) or CS. The eventual decision depends on several factors, of which these are especially significant: the obstetrician’s clinical judgment regarding the cause of arrest of descent, the appropriateness of the intervention in the given clinical context, the obstetrician’s proficiency in carrying out either intervention and maternal opinion. In some cases, both interventions may be attempted, such as CS after a failed attempt at ID. An increase in the rates of emergency CS performed specifically in the second stage of labour has been documented,(8-11) reflecting the decreasing popularity of attempted ID as a first-line intervention in patients with a prolonged second stage of labour.
Although several studies have been done to compare the prevalence of maternal and neonatal morbidity and mortality between second-stage CS and ID,(12) similar data is limited in the Asian population, where maternal height and pelvic dimensions, which influence the likelihood of cephalopelvic disproportion (CPD), are significantly different.(13-15) These differences are an important consideration, as a clinical diagnosis of CPD precludes the use of ID, hence influencing the rates of IDs and second-stage CSs. Additionally, no randomised controlled trial has been carried out to compare the outcomes of both types of interventions.
The aims of this study were: (a) to compare emergency second-stage CS and ID performed at Singapore General Hospital (SGH), Singapore, specifically for poor progress in the second stage of labour over a three-year period from 2010 to 2012; and (b) to determine the rates of IDs compared to CSs for poor progress in the second stage of labour, factors influencing the eventual mode of delivery, and if there was a difference in maternal and neonatal outcomes between both groups.
METHODS
Patients were identified via the labour ward database maintained at SGH. We included women with singleton vertex pregnancies who required either an emergency CS at full dilatation for clinically diagnosed CPD, or ID for prolonged second stage of labour between 1 January 2010 and 31 December 2012. For nulliparous women, prolonged second stage was defined as greater than three hours with an epidural and greater than two hours without an epidural; in multiparous women, it was defined as greater than two hours with an epidural and greater than one hour without an epidural. Medical records for these patients were obtained and appropriate data was extracted.
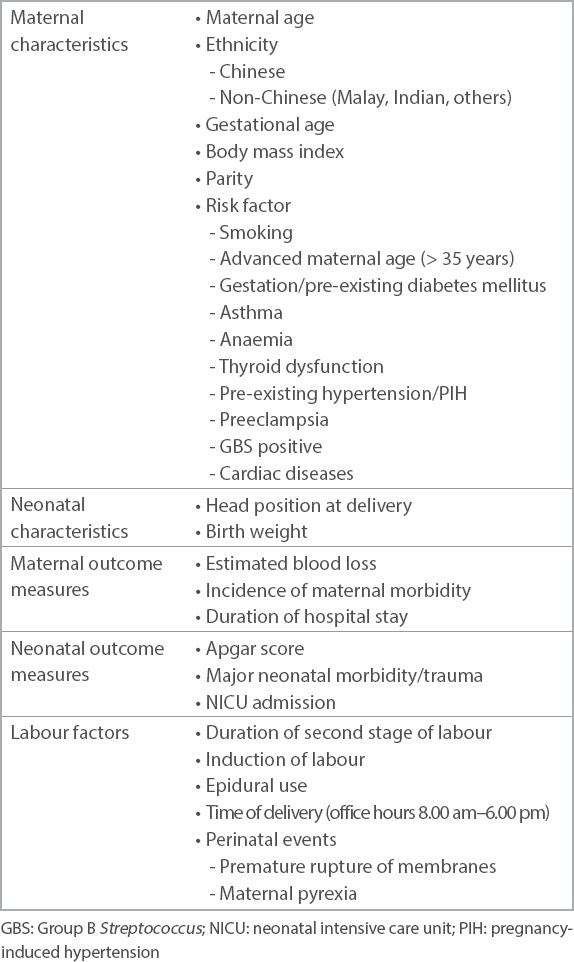
We considered maternal and neonatal characteristics and outcome measures, as well as labour factors including presence of any perinatal complications. Maternal characteristics included maternal age, ethnicity, gestational age, body mass index (BMI), gravidity, parity, and presence of any documented risk factors such as smoking, advanced maternal age (defined as maternal age more than 35 years), gestational and pre-existing diabetes mellitus, asthma, anaemia, maternal hyper- or hypothyroidism, pre-existing hypertension, pregnancy-induced hypertension or preeclampsia, cardiac disease and Group B Streptococcus positivity. Maternal outcome measures that were considered were estimated blood loss, incidence of maternal morbidity and length of hospital stay. Neonatal characteristics included head position and fetal weight, while neonatal outcome measures comprised neonatal intensive care unit (NICU) admission, neonatal trauma and Apgar score at five minutes. Labour factors considered included duration of second stage, spontaneity of labour, epidural use, instrument type in IDs, perinatal complications (e.g. premature rupture of membranes and maternal pyrexia) and time of delivery, with office hours taken to be 8.00 am–6.00 pm (
Table I
Maternal and neonatal demographics.
Comparative analysis of categorical and continuous variables was performed using chi-square and Mann-Whitney U tests, respectively. A p-value < 0.05 was considered statistically significant. SPSS Statistics version 23.0 (IBM Corp, Armonk, NY, USA) was used for all analysis.
The study was exempted from formal ethics approval by the SingHealth Centralised Institutional Review Board, the main body involved in approving, monitoring and review of any biomedical and behavioural research in our institution involving humans.
RESULTS
A total of 4,426 deliveries were performed, of whom 253 (5.7%) patients required intervention for a prolonged second stage of labour. ID was attempted in 187 patients, while 66 patients were directly listed for emergency CS. Of the 187 attempted IDs, five were unsuccessful and CS was eventually performed, resulting in an instrumental delivery failure rate of 2.7%. Hence, a total of 182 women underwent delivery by ID and 71 women by CS (
Fig. 1
Flowchart shows successful ID attempts in prolonged second stage of labour. ID: instrumental vaginal delivery
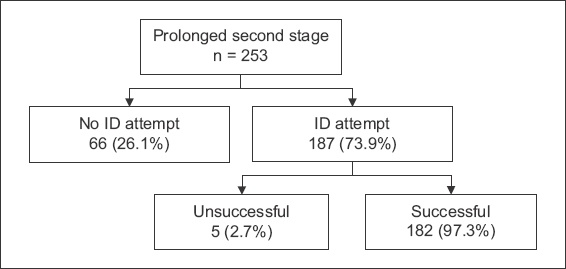
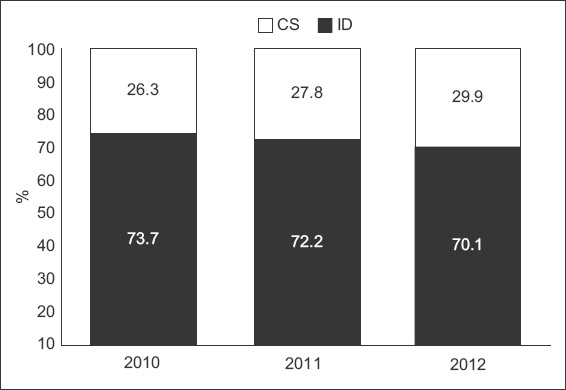
Fig. 2
Graph shows the changes in rates of Caesarean section (CS) and instrumental vaginal delivery (ID) performed for prolonged second stage of labour from 2010 to 2012.
There were no significant differences in maternal BMI (p = 0.288), age (p = 0.462), parity (p = 0.831), gestational age (p = 0.899) at delivery, or risk factors between both groups. However, there was a significantly higher rate of CS deliveries among Chinese compared to non-Chinese mothers (p = 0.007) (
Table II
Maternal demographics.
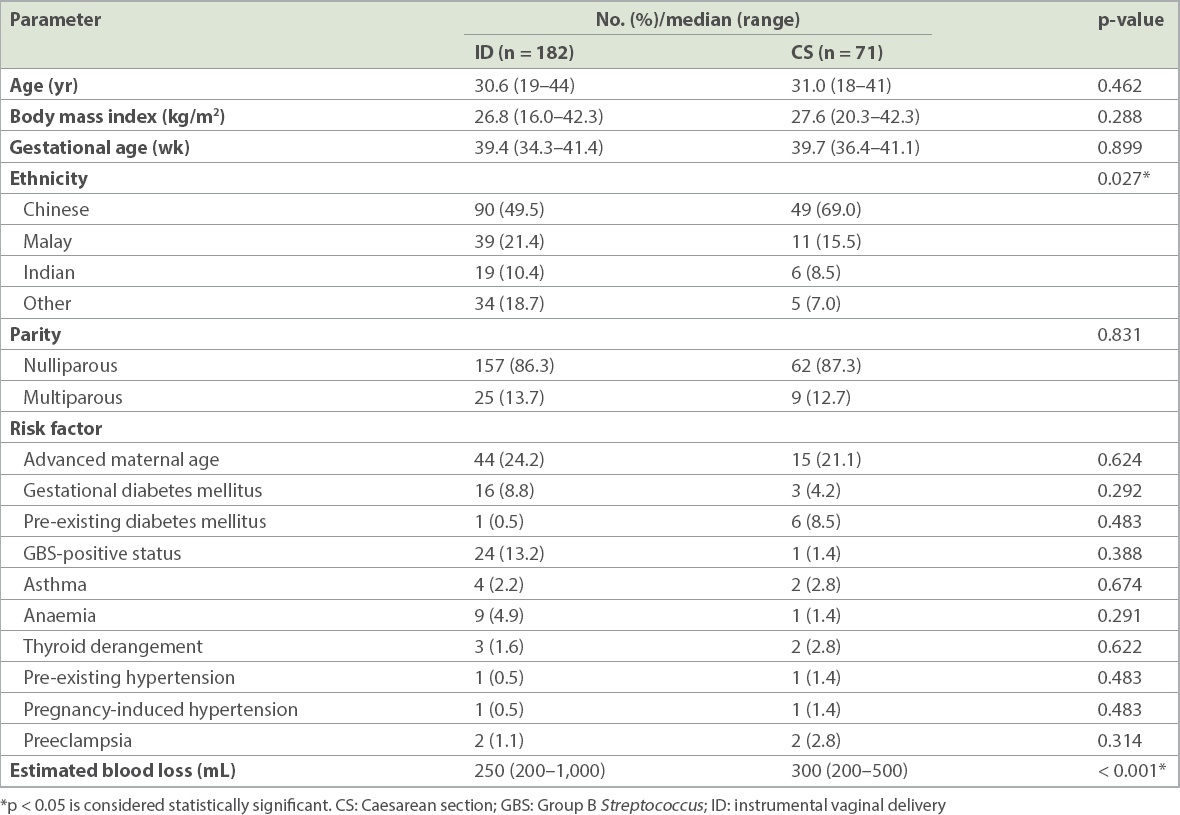
Table III
Neonatal characteristics and outcomes.
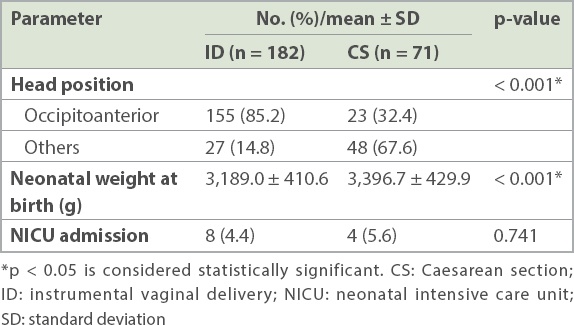
Table IV
Comparison of labour and delivery outcomes.
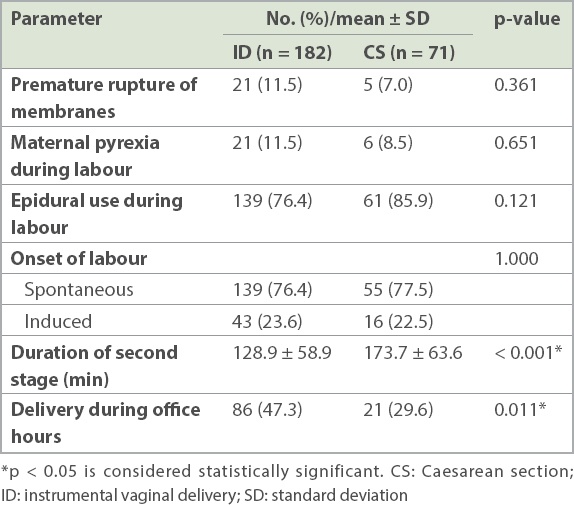
With regard to outcomes, mothers in the CS group had significantly higher estimated blood loss (p < 0.001) (
DISCUSSION
In keeping with worldwide trends,(16-19) the percentage of second-stage CSs in our institution showed a year-on-year increase with a corresponding decrease in the percentage of IDs, reflecting a growing reluctance to perform ID. There is limited literature available regarding the incidence of arrest of descent, and reported figures range widely, from 1.7% in a retrospective study by Feinstein et al(20) to 11.5% as reported by Leushuis et al.(21) The reported incidence in our study lies in between these figures, at 5.7%. This difference has been attributed to the proportion of nulliparous women included in each study, in which a higher percentage of nulliparous women is associated with a higher incidence of arrest of descent; however, this is unlikely to be the only contributing factor, as the proportion of nulliparous women in our study was higher than in both previously mentioned studies, at 86.6%, compared to 21% in Feinstein et al(20) and 45% in Leushuis et al.(21) The incidence of CS for prolonged second stage was marginally higher in our study (28.0% vs. 14.8% in Leushuis et al).(21) In cases where ID was the intervention of choice, failure rates were low compared to other reported figures,(22) which could either reflect operator competence or a conservative approach in attempting ID.
In our study, significant factors affecting the eventual mode of delivery were maternal ethnicity, duration of second stage of labour, neonatal weight and head position. Ethnically Chinese mothers were more likely to undergo CS if they required intervention in the second stage. This difference could be a result of maternal choice rather than intrinsic differences in factors such as body habitus. BMI was not shown to be a contributing factor, as the median BMI of Chinese women was significantly lower than that of non-Chinese women (26.29 vs. 28.59; p = 0.002), and only higher BMI is associated with increased risk of CS.(22) This indicates the presence of other factors influencing the final choice of intervention in Chinese mothers. Differences in the rates of both elective and emergency CSs among various ethnic groups have also been reflected in other studies, but have never been fully accounted for.(23-25) Further studies would be useful in determining the reasons for this disparity in CS rates.
In our study, the duration of the second stage of labour was longer in the CS group compared to the ID group. This is possibly due to the fact that patients who experienced a prolonged arrest of descent were more likely to be diagnosed with CPD and hence undergo CS rather than ID. The significant differences in fetal head position between both groups are similarly unsurprising, as fetuses presenting in the occipitoanterior position are more amenable to ID due to easier positioning of the instrument. Although malposition is not an absolute contraindication for ID, it has been associated with higher ID failure and complication rates,(22) which might have affected the obstetrician’s choice of CS over ID. In our study, babies born in the CS group tended to be heavier, a finding that was consistent with the available literature.(26) As the risk of CPD rises with increasing fetal size (with fetal weight as a surrogate measure), this suggests that the attending obstetricians in our hospital had sound clinical judgment in making a diagnosis of CPD and hence choosing CS over ID.
Notably, our study also found that a larger proportion of IDs were performed during office hours, when consultant obstetricians were present on-site and able to personally manage women experiencing a prolonged second stage of labour. Our findings are similar to those of other centres, where after-hour consultant presence in the maternity ward resulted in higher ID rates and lower rates of operative deliveries.(27,28) We may infer that non-consultant-grade staff generally lack either the skill or confidence in attempting IDs when compared to consultant obstetricians, and are more likely to prefer CS in the event of prolonged second stage. However, the declining rates of ID worldwide perpetuate a vicious cycle in which there are fewer opportunities for obstetric trainees, further compounding their lack of confidence and skill. The Royal College of Obstetricians and Gynaecologists (RCOG) recently proposed a 24-hour consultant cover on maternity wards,(29) given the growing complexity of obstetric cases and increase in operative birth rates. Although such a move would benefit maternal care, it does not necessarily lead to enhanced training and supervision for trainees. Furthermore, studies evaluating the impact of after-hour consultant cover have failed to demonstrate a significant difference in neonatal and maternal morbidity.(27)
Another important factor contributing to a reluctance to attempt ID could be the increasingly litigious medicolegal climate affecting the medical community,(30) especially in obstetrics. As previously described succinctly by Chou: “A perfect baby is the expectation of all parents, and a perfect outcome is the mission of obstetrics.”(31) Moreover, litigation rates have always been comparatively higher in obstetrics compared to other medical specialties,(32,33) resulting in obstetricians adopting a more conservative approach in the face of unforeseen clinical events. As such, obstetricians might have developed a preference for emergency CS as the intervention of choice for a prolonged second stage of labour in order to avoid the potential risk of ID failure.
For anticipated difficult IDs, a trial of ID in the operating theatre (ToD) has been proposed as a viable alternative to CS, such that immediate recourse to CS is available in the event of failure. This is not practised in our institution and little data on the prevalence of ToD is available for comparison. Available figures range from 2% to 26%.(34,35) The RCOG Green-top Guidelines for operative vaginal delivery (2011) presented a list of factors that are predictive of difficult IDs, including elevated maternal BMI, estimated fetal weight over 4,000 g, fetal occipitoposterior position and mid-cavity deliveries, proposing that such deliveries should be considered for ToD, purportedly to reduce unnecessary CSs. This was based on the premise that fetal morbidities can be attributed to a delay between failed operative vaginal delivery and CS. However, several studies have highlighted the issue of a prolonged decision-to-delivery interval for cases of ToD due to the time taken for preparation and transfer.(34,35) Interestingly, a Cochrane review by Majoko et al(36) reported an absence of randomised controlled trials comparing ToD with immediate CS for anticipated difficult assisted births, and therefore a lack of evidence to suggest that neonatal outcomes are comparable in both groups. The overall low rates of ToD, thus, not only reflect changing attitudes towards ID in general, but could also be attributed to the potentially increased risk of neonatal morbidity associated with prolonged decision-to-delivery intervals.
A comparison of maternal and neonatal outcomes showed that there were no statistical differences in neonatal outcomes between the ID and CS groups. All neonates included in our study had five-minute Apgar scores of 7 or more, which was considered reassuring in a policy statement by the American Academy of Paediatrics’ Committee on Fetus and Newborn.(37) There were also no differences in incidence of NICU admission at birth. Maternal outcomes were significantly different for estimated blood loss, with CS resulting in a marginally larger amount of blood loss. However, there were no cases of major haemorrhage, and the slight difference in blood loss is likely to be clinically insignificant. Existing studies comparing the differences in outcomes between ID and CS in the second stage of labour as well as those investigating outcomes of CS performed in the second stage of labour report similar results: a generally low incidence of CS was associated with increased morbidity in the form of higher blood loss, longer duration of hospital stay, and uterine tear.(38,39)
Our study was limited by its retrospective nature and relatively small sample size. Documentation was not always sufficiently detailed and may have affected the accuracy of our findings. However, our results provide insight into obstetric practices in the Asian setting, which is scarcely represented in the limited available literature comparing ID and CS in the second stage of labour. Large prospective studies are required to better determine if one option has a significant advantage over the other in ambiguous clinical situations, information that would be invaluable in clinical decision-making.
In conclusion, this study found that more than one in four parturients at full dilatation requiring intervention for prolonged second stage had an emergency CS. The frequency of failed instrumentation was low and babies in the CS group were larger, suggesting sound clinical judgment in diagnosing CPD at full dilatation. However, there were no attempts at ToD, and a higher incidence of CS after hours without in-house consultants suggests trainee reluctance to attempt instrumental delivery. This could indicate cautiousness in an increasingly litigious medicolegal environment as well as decreased clinical experience. Differences in neonatal and maternal outcomes between both intervention methods were also found to be clinically insignificant.


