Abstract
INTRODUCTION
Empathy and burnout are two entities that are important in a physician’s career. They are likely to relate to each other and can be heavily influenced by surrounding factors, such as medical education, local practices and cultural expectations. To our knowledge, empathy and burnout studies have not been performed in Singapore. This study was designed to evaluate empathy and burnout levels using the Jefferson Scale of Physician Empathy (JSPE) and Maslach Burnout Inventory (MBI) among residents in Singapore, and compare them with the United States (US) literature.
METHODS
The JSPE, MBI and a self-designed questionnaire were completed by 446 trainees at a residency-sponsoring institution in Singapore.
RESULTS
Residents in Singapore had lower empathy and higher rates of burnout compared to US literature. Physician empathy was associated with burnout: residents with higher empathy scores had higher personal accomplishment (p < 0.001, r = 0.477, r2 = 0.200); and lower emotional exhaustion (p < 0.001, r = 0.187, r2 = 0.035) and depersonalisation (p < 0.001, r = 0.321, r2 = 0.103) scores.
CONCLUSION
Residents in Singapore had lower empathy and higher burnout scores compared to the US literature. Further research into the underlying cause is imperative to guide intervention.
INTRODUCTION
Physician empathy is a cognitive attribute that involves the ability to understand a patient’s inner experiences, feelings and concerns, combined with an ability to communicate this understanding and an intention to help.(1) Empathy is an innate characteristic that develops from an early age.(2) Physicians who are highly empathetic tend to display multiple positive attributes, such as dutifulness, moral reasoning and clinical competence,(3) as well as better outcomes, such as lower rates of malpractice litigation,(4) enhanced patient satisfaction,(4,5) better physician-patient relationships(6) and, ultimately, better clinical outcomes.(7) Physician empathy may fluctuate over time and is influenced by working conditions and circumstances.
Studies have recognised that many physicians experience professional burnout, as characterised by loss of enthusiasm toward their work (emotional exhaustion [EE]), feelings of cynicism (depersonalisation [DP]) and a low sense of personal accomplishment (PA).(8-10) Resident burnout is a major problem, and burnout prevalence rates among United States (US) residents have been found to be in the range of 47%–70%.(11-13) High levels of burnout is an issue that can be detrimental to clinical practice, eroding professionalism, influencing quality of care and increasing risk of medical errors.(9) On a personal level, burnout may also contribute to broken relationships(14) and mental health issues, such as substance abuse and suicidal tendencies.(15)
The relationship between empathy and burnout is complex and has been studied previously. There is evidence that burnout hampers empathy. Physicians who experience exhaustion and burnout are often depersonalised in social interactions and less capable of demonstrating empathy, such as standing in the patient’s shoes and listening empathetically.(16,17) Interestingly, the reverse effect of empathy on burnout is less clear. Studies have demonstrated that empathy can create as well as prevent burnout. ‘Compassion fatigue’ is an example of how over-relating to a patient’s suffering may lead to emotional exhaustion among physicians.(18) On the other hand, empathy is often associated with job satisfaction, which protects physicians from emotional exhaustion.(19) Again, to the best of our knowledge, the association between empathy and burnout has not been studied in Singapore.
Singapore is a modern society that is highly competitive, with long working hours and high job stress. Moreover, traditional values in society and its expectations of physicians may lead to excessive emotional exhaustion and physician burnout. Medical students in Singapore have been shown to be less empathetic than their counterparts from the US, although they were relatively more empathetic compared to counterparts from East Asia.(20) Similarly, nurses in Singapore have intermediate levels of burnout when compared to their peers from China or the United Kingdom (UK).(21) Singapore likely represents a middle ground, with a confluence of Eastern and Western cultures, and is a unique context to evaluate empathy and burnout.(20) This study was conducted to evaluate empathy and burnout among residents in Singapore. We hypothesised that residents in Singapore have high levels of burnout and low levels of empathy compared to the US literature.
METHODS
Our cross-sectional study cohort included 446 residents from SingHealth Residency, out of the 879 eligible residents at the time of the survey. Residents were from 34 different programmes and training sites that spanned three general hospitals (Singapore General Hospital, KK Women’s and Children’s Hospital and Changi General Hospital), five National Specialty Centres and nine community clinics in Singapore.
We used the Jefferson Scale of Physician Empathy for physicians and health professionals (JSPE-HP; referred to as JSPE henceforth)(1,22) and Maslach Burnout Inventory-Human Services Survey version, distributed by Mind Garden© (MBI-HSS; referred to as MBI henceforth),(23,24) as tools to measure empathy and burnout levels, respectively. We have previously published findings on the validity and reliability of the JSPE in Singapore.(20) The JSPE included 20 Likert-type items answered on a 7-point scale (1 = strongly disagree; 7 = strongly agree) with a possible score range of 20–140. The tool incorporates three factors: perspective-taking, compassionate care and standing in the patient’s shoes. This is consistent with the concept of a multidimensionality notion of empathy.(25) The MBI included 22 Likert-type items answered on a 6-point scale, which is subdivided into three scales: emotional exhaustion (EE; nine items intended to measure EE; possible score range 0–54); depersonalisation (DP; five items intended to measure perceptions of impersonal, non-appreciative responses by others for providing services or help; possible score range 0–30); and personal accomplishment (PA; eight items measuring perceptions of competence, and successful academic and professional achievement; possible score range 0–48). Clinically significant burnout was defined as having a high subscore on any subscale.(23) We also incorporated a self-designed questionnaire, which included basic demographic information and 21 Likert-type items answered on a 5-point scale to measure structural and personal factors that affected participants’ residency training (Appendix).
The study was given an institutional review board waiver by the SingHealth Centralised Institutional Review Board. It was conducted over a five-month period between 1 January 2015 and 31 May 2015. The questionnaire was administered online, as a packet of three instruments (JSPE, MBI and self-designed questionnaire), via the New Innovations client (New Innovations Inc, Uniontown, OH, USA). Two weekly email reminders were sent to non-respondents.
Participation was voluntary and residents’ information was anonymised with a coded identifier. An information technology analyst and a programme executive who were not involved in data analysis maintained the master list. The data was password-protected.
Statistical analyses were performed using IBM SPSS Statistics version 20.0 (IBM Corp, Armonk, NY, USA). Cronbach’s alpha was calculated to evaluate the internal consistency reliability of the tool. The JSPE scores of respondents were analysed by year of residency using analysis of variance with Bonferroni correction. Gender, specialty choice, marital status, alcohol use and employment of domestic help were analysed using two-tailed t-tests. Linear regression was used to examine the relationship between empathy and the individual burnout components of the MBI.
RESULTS
Of the 879 eligible residents, 446 (50.7%) volunteered and completed the self-assessment questionnaire. The demographic characteristics for this sample are shown in
Table I
Baseline characteristics of enrolled residents (n = 446).

Cronbach’s alpha coefficient for the JSPE was 0.870, while that for the MBI was 0.848. This demonstrated that both tools had an acceptable level of internal consistency and reliability. The overall mean JSPE score for our cohort was 104.9 ± 13.2. We did not observe significant differences in overall JSPE empathy scores, or its individual subsets, between residents at different years of training (
Table II
JSPE score, MBI and individual factors in the construct of empathy and burnout for residents.
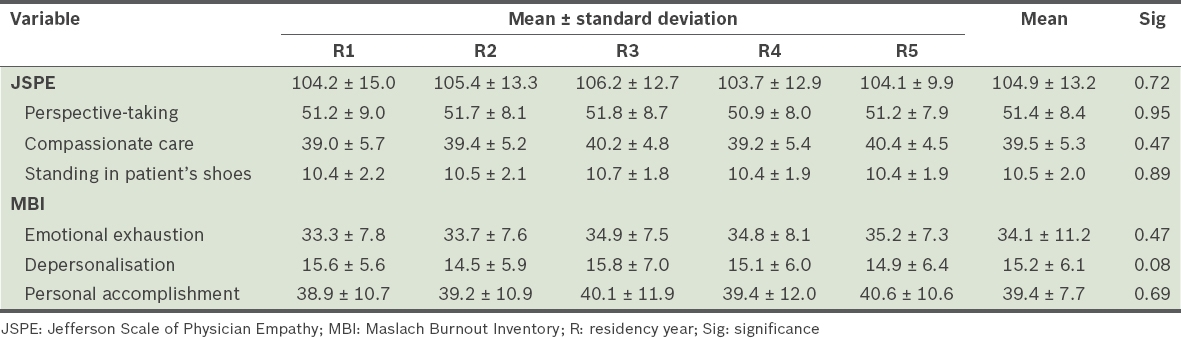
As measured by the MBI, mean scores of EE, DP and PA were 34.1 ± 11.2, 15.2 ± 6.1 and 39.4 ± 7.7, respectively. Maslach et al described high rates of burnout among physicians as scores of EE ≥ 27, DP ≥ 11 and PA ≤ 33.(23) Using this reference range, we found that 360 out of 446 (80.7%) residents had burnout in at least one of the domains. Similar to the empathy scores, there were no significant differences in the rates of burnout and its components between residents at different years of training (
Residents with higher empathy scores were associated with lower EE (p < 0.001, r = 0.187, r2 = 0.035) and DP (p < 0.001, r = 0.321, r2 = 0.103), and higher PA (p < 0.001, r = 0.477, r2 = 0.200). For every unit increase in JSPE, there was a 0.158-point and 0.149-point decrease in EE and DP, respectively, and 0.26-point increase in PA.
DISCUSSION
The main objectives of this study were to: (a) assess the levels of empathy and burnout among residents in Singapore; and (b) compare findings with the US literature. Our findings suggested that residents in Singapore have lower empathy and higher rates of burnout compared to US studies. The mean empathy score for our cohort was 104.9 ± 13.2, which was lower than that of physicians in the US (empathy score 120 ± 15.6).(1) Rates of burnout and mean MBI scores were also significantly higher than those in the published data.(8,26) The prevalence of burnout in our cohort was 80.7%, significantly higher than in the US (range 47%–70%).(11-13) Mean burnout scores in our cohort (EE: 34.1 ± 11.2; DP: 15.2 ± 6.1; PA: 39.4 ± 7.7) were also significantly higher than the respective median US scores (EE 21.0; DP 5.0; PA 42.0).(8)
Our findings also suggest that physician empathy was correlated with burnout. Among the three subscales of the MBI, empathy was positively correlated with PA but inversely associated with EE and DP, the other indicators of burnout. Possible explanations for this include: (a) burnout reduces empathy; and (b) empathy prevents burnout (‘job satisfaction’).(27) The relationship between empathy and burnout is complex, but further investigation on the direct link between them was beyond the scope of this study.
Our data indicated that the relative contribution of empathy and burnout to each other may not be very large. The r2 values derived from logistic regression analysis (EE: r2 = 0.035; DP: r2 = 0.103; PA: r2 = 0.200) were small, suggesting that while empathy and burnout are related, there remains a large undefined component in their combined construct that is yet to be elucidated. We opine that empathy and burnout may be manifestations of the same personal-emotional construct. Further studies would be useful to understand the intricacies of empathy and burnout in the development of a resident’s professionalism.
An interesting observation in our study was that empathy and burnout scores remained stable during residency training. This was in contrast to studies on US residents, where there was a trend of declining empathy as well as increasing fatigue and anger during the course of their training.(28) The exact cause of this is unclear, and there may perhaps be certain cultural factors that are protective toward empathy decline and burnout. Alternatively, empathy decline and burnout may happen earlier even before residency, during training in medical school, and levels may have ‘bottomed-out’ by the time students graduate. In order to further elucidate this, we are continuing our longitudinal study from medical school to residency training.
To our knowledge, this was the first study in Singapore to evaluate empathy and burnout among residents. Our findings suggest that empathy is lower and burnout higher among our residents when compared to US residents.(1,11-13,29) This is likely a reflection of multiple factors, ranging from medical education to work factors, such as hospital work-hours and policies, as well as societal expectations on physicians. Nevertheless, this issue is alarming, as empathy decline and high burnout can have serious repercussions for physicians’ well-being and adversely affect quality of patient care.(9)
The US literature was used for our comparison because the majority of empathy and burnout literature on residents was based in the US. We also felt that the two training systems, that is, the local residency programme and the strict guidelines from the Accreditation Council for Graduate Medical Education in the US, were similar. This may allow us to hypothesise that reasons unrelated to training, such as local practices and cultural differences, were responsible for the disparity in results. Further examination of the hypothesis was, however, beyond the scope of the current study.
The main limitation of the present study was that it was conducted at a single sponsoring institution, restricting the generalisability of our results. Non-response may also have caused sampling errors and affected the results. We were unable to compare non-responders with responders, as the results were coded and anonymised, and the investigators were blinded. Nevertheless, our response rate was 50.7%, similar to the typical rate of 52% reported for physician surveys.(30) Cross-sectional investigations have shown no significant differences between responders and non-responders in physician survey studies.(31) Finally, our questionnaire examined residents’ recollections of experiences and therefore may have been susceptible to recall bias.
In summary, our findings suggest that empathy is lower and burnout higher among residents in Singapore when compared to their US counterparts. We also described the association between empathy and burnout. Further research into the underlying cause of this association is necessary in order to plan protective interventions.
SMJ-59-50-appendix.pdf
ACKNOWLEDGEMENTS
This study was supported by an education research grant from the Academic Medicine Education Institute (AM.EI), Duke-NUS Medical School, Singapore. We would also like to thank Prof Sandy Cook, Senior Associate Dean, AM.EI, who provided us with useful suggestions, Mr Samad Bin Asad, SingHealth Information Technology Department, who anonymised residents’ data, programmed the electronic questionnaire and maintained the master list, Mr Shaw Yang Chia, statistician at National Heart Centre Singapore, who assisted in looking through the statistical analyses, and Ms Jeannie Lum, Programme Executive, SingHealth Cardiology Senior Residency Programme, who helped to liaise with other programme executives in the running of this study.


